Skipping your first mammogram can raise your risk of dying from breast cancer by 40% over 25 years due to delayed detection. That single statistic reframes what many people treat as a minor calendar reminder into something far more serious. Health screening is the practice of testing people who feel perfectly fine to catch disease before it causes symptoms. In this article, you will learn what screening actually is, which tests matter most, how effective they are, and how to build a screening plan that fits your life.
Table of Contents
- Defining health screening: What it is and why it matters
- Common types of health screening tests
- Health screening effectiveness and participation rates
- Balancing benefits and harms: When health screening makes sense
- How to apply health screening to your own preventive care
- Connecting health screening with professional care
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Early detection saves lives | Health screening can uncover serious conditions before symptoms appear, leading to better treatment and outcomes. |
| Choose screenings by risk | Not all screenings are equal; tailor your choices based on age, risk factors, and expert guidelines. |
| Balance benefits and harms | Understand the risks of false positives and overdiagnosis, and discuss screening decisions with your provider. |
| Participation impacts health | Rates of screening uptake are linked to population health and can vary based on equity and access. |
| Professional guidance matters | Consult health professionals to set a personalized screening schedule for preventive care. |
Defining health screening: What it is and why it matters
A lot of people confuse screening with getting a diagnosis. They are not the same thing. Health screening is the use of tests or procedures to detect diseases or health conditions in people who have no symptoms, with the goal of early detection, prevention, or better treatment outcomes. Diagnosis, by contrast, targets symptomatic individuals who already show signs of illness. Screening comes first, and it casts a much wider net.
Understanding this difference matters because it changes how you think about your own health. You do not need to feel sick to benefit from a screening. In fact, the whole point is to act before you feel anything at all. If you want a broader picture of how this fits into outpatient procedures, it helps to see screening as one layer of a larger preventive system.
"Screening tests must meet established criteria: the condition must be serious, the test must be reliable, and effective treatment must be available. Voluntary participation and informed consent are non-negotiable."
Here is what good screening programs are designed to do:
- Catch disease at its earliest, most treatable stage
- Reduce mortality and long-term complications
- Identify risk factors before they become full conditions
- Support informed, voluntary health decisions
- Contribute to medical wellness as a long-term strategy
Common types of health screening tests
Once you understand what screening is, the next question is: what tests are actually out there? The answer depends on your age, sex, and personal risk profile. Common methodologies include blood tests for cholesterol and glucose, imaging like mammograms and low-dose CT scans, Pap and HPV tests for cervical cancer, colonoscopy for colorectal cancer, and physical exams that measure blood pressure and body mass index.
Here is a quick comparison of major screening tests and what they target:
| Screening test | Condition detected | Recommended group |
|---|---|---|
| Mammogram | Breast cancer | Women 50 to 74 |
| Pap/HPV test | Cervical cancer | Women 21 to 65 |
| Colonoscopy | Colorectal cancer | Adults 45 to 75 |
| Low-dose CT | Lung cancer | High-risk adults 50 to 80 |
| Blood pressure check | Hypertension | All adults |
| Fasting glucose | Diabetes | Adults 35 to 70 with overweight |
USPSTF and CDC guidelines recommend specific screenings based on age and risk, and these recommendations are updated regularly as new evidence emerges. You can explore screening test options in more detail to match tests to your personal profile.
For women, dedicated programs like women and child checkups and executive women screening cover the full range of age-appropriate tests. Men have equally tailored options through executive men screening, while basic health checkups offer a solid starting point for anyone new to preventive care.
Pro Tip: Before your next appointment, write down your age, any family history of chronic disease, and your lifestyle habits. Bring that list and ask your provider which screenings from the health checkup services catalog apply to you specifically.
Health screening effectiveness and participation rates
Knowing which tests exist is one thing. Understanding how well they actually work is another. The data is encouraging, but participation gaps remain a real problem.

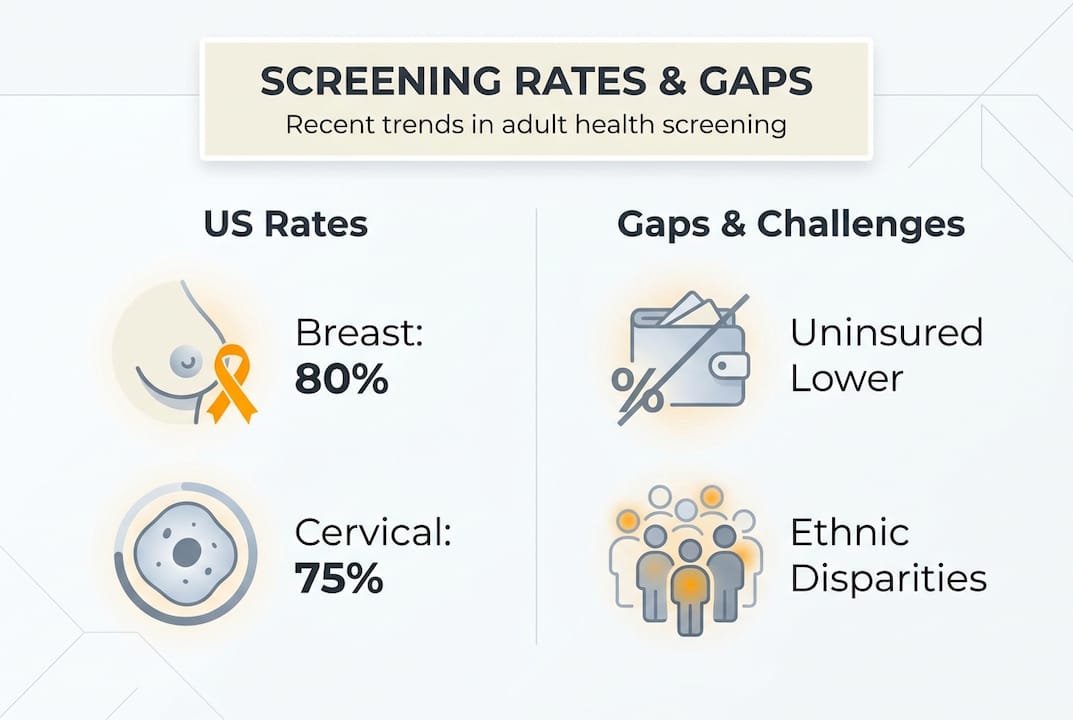
In 2023, US screening rates showed that 80% of eligible adults were up to date on breast cancer screening, 75.4% on cervical cancer screening, and 67.4% on colorectal cancer screening. However, among adults aged 45 to 49, the colorectal cancer screening rate dropped sharply to just 37.1%, a group that only recently became eligible under updated guidelines.
| Screening type | Overall rate (2023) | Notable gap |
|---|---|---|
| Breast cancer | 80% | Lower in uninsured women |
| Cervical cancer | 75.4% | Lower in rural areas |
| Colorectal cancer | 67.4% | Only 37.1% in ages 45 to 49 |
The picture for abdominal aortic aneurysm (AAA) screening in the UK is striking. Among men aged 65 and older, the program reduced emergency AAA admissions by more than two thirds, prevalence fell from 1.2% to 0.8%, and elective surgery survival reached 98.5%. That is what a well-run screening program can achieve.
Equity is a persistent challenge. People in lower-income areas, those without insurance, and individuals from certain ethnic groups consistently show lower participation rates. Improving uptake in these populations is one of the most important levers for better public health outcomes. Supporting holistic medical wellness means addressing access, not just awareness.
Balancing benefits and harms: When health screening makes sense
Screening is not a risk-free activity. That might surprise you, but it is important to understand before you agree to any test.
The benefits are real and well-documented. Colorectal cancer screening can remove precancerous polyps before they become cancer. Breast and cervical cancer screening catches tumors early when treatment is most effective. For these conditions, benefits outweigh harms according to established guidelines. But the picture is not always clean.
Here is what the risks look like in practice:
- False positives trigger anxiety and lead to follow-up tests that may be unnecessary
- Overdiagnosis means detecting a cancer that would never have caused symptoms or death
- Procedure complications are rare but real, especially with invasive tests like colonoscopy
- For breast cancer, some estimates suggest 3 cases are overdiagnosed for every 1 life saved
"Individual risk-benefit assessment is essential. What works at the population level may not be the right choice for every person."
Population-level cardiovascular screening, for example, has shown limited effectiveness in some studies, while cancer screening remains strongly supported for specific age groups and risk profiles. The USPSTF framework grades each recommendation based on the strength of evidence, which helps both providers and patients make better decisions.
Pro Tip: Before agreeing to any screening, ask your provider two questions: "What is the chance this test gives a false positive?" and "What would we do differently if the result is positive?" Those answers will tell you a lot about whether the test is right for you.
For a closer look at where common screening pitfalls occur, reviewing real-world examples can help you ask sharper questions at your next visit.
How to apply health screening to your own preventive care
Understanding the theory is useful. Putting it into practice is what actually protects your health. Here is a step-by-step approach to building a screening schedule that works for you.
- Know your baseline. Write down your age, sex, family medical history, and any chronic conditions. This is the foundation of any personalized screening plan.
- Check current guidelines. Look up what national bodies like the USPSTF recommend for your age and sex. These are updated regularly, so check them every year or two.
- Talk to your provider. Bring your baseline information and ask which WHO-criteria screenings apply to you. A good provider will explain the evidence, not just hand you a referral.
- Ask about your individual risk. Family history, lifestyle, and ethnicity can all shift your risk profile above or below the population average. Some people need earlier or more frequent screening.
- Give informed consent. You have the right to understand what a test involves, what the results mean, and what happens next. Voluntary, informed participation is a core principle of ethical screening.
- Schedule and track. Put your next screening date in your calendar. Gaps in screening are one of the most common reasons for late-stage diagnoses.
- Revisit your plan annually. Your risk profile changes as you age. What was not recommended at 40 may be essential at 50. Build holistic care and prevention into your yearly health review.
Connecting health screening with professional care
Reading about screening is a great first step. Acting on it is what makes the difference. At Globallmed, our private outpatient clinic in Macau is designed to make that step as straightforward as possible.

Our medical clinic department offers personalized consultations where our clinical team reviews your health history and recommends the screenings that actually fit your profile. We do not apply a one-size-fits-all approach. Whether you are looking for a first-time checkup or a more targeted program, our women and child screening services and broader checkup packages are built around evidence-based guidelines and delivered by qualified professionals. Book a consultation and take the guesswork out of preventive care.
Frequently asked questions
How often should I get health screenings?
Frequency depends on your age, sex, medical history, and risk factors. USPSTF guidelines provide age-specific timelines, but your provider can adjust these based on your personal profile.
Are health screenings always safe and accurate?
Most screenings are safe, but false positives and overdiagnosis are real risks. Always discuss the potential harms alongside the benefits with your provider before agreeing to a test.
Does health screening really help prevent disease?
Screening is most effective for certain cancers and select conditions. Benefits outweigh harms for guideline-supported tests, but effectiveness varies by condition and individual risk.
What happens if I miss a recommended screening?
Missing a screening can lead to later-stage detection and worse outcomes. Non-participation in mammography is linked to 40% higher breast cancer mortality over 25 years, which shows how much timing matters.
